This Journal covers important information on vitamin K2, a fat soluble vitamin of the vitamin K family, which prevents calcium from being deposited in peripheral tissues, and assists its deposition in bone and teeth. The points registered below are worth knowing about as you grow your vitamin K2 into health promoting levels.
In addition to preventing coronary artery and heart valve calcification, vitamin K2 prevents calcification in other tissues such as joints and bone spur sites. It is also an anti-inflammatory agent. Furthermore, vitamin K2 deficiency is now being linked to prostate cancer, diabetes, and the cerebral vascular changes and plaque formation dynamics which accompany dementia processes.
Vitamin K2 deficiency in our culture is likely to be more ubiquitously common than vitamin D deficiency. Deficiencies of these vitamins help account for the all too common incidence of calcified atherosclerotic blood vessels, heart valves, hypertension, heart failure, calcified arthritic joints, and other calcified soft tissues. Since all disease processes have their origins in inflammation chemistry, the list of diseases linked to vitamin K2 deficiency will grow.
Vitamin K2 functions in cardiovascular health and in bone mineralization. By preventing the deposition of calcium in the lining of the blood vessels and shuttling it into the bone matrix, vitamin K2 helps prevent vascular occlusions due to atherosclerosis.
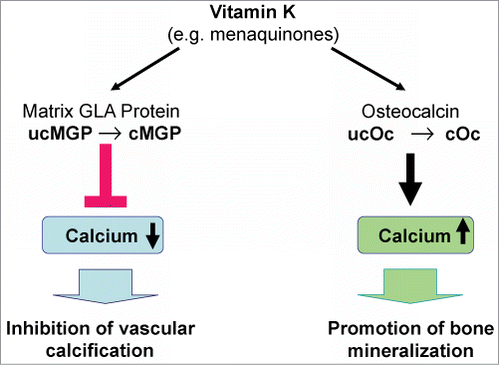
Vitamin K2 functions with vitamin D to produce and activate Matrix Gla-protein (MGP) which functions in the elastic fibers of arterial lining to help protect arteries by inhibiting the calcification of vascular smooth muscle.
Back in my surgery days of operating on calcified blood vessels I used to wonder how an entire abdominal aorta or an iliac artery or a femoral artery or a popliteal artery or a carotid artery could become completely replaced by calcium deposition. Many of the blood vessels I operated on were entirely fossilized by an aggressive calcification process. While cigarette smoking and oxidized cholesterol particles are major contributing factors, there would have to be other dynamics at play to account for such alarming pathology.
These blood vessels were as hard as rock and usually could not be operated on. A surgeon could not drive a suture through these vessel walls. The only solution was to bypass the calcified portion with some sort of graft (Gortex, Dacron, or autologous reversed veins), if that was even possible.
In cases where the abdominal aorta and iliac arteries were ossified, the only solution was to tunnel a long graft from one of the axillary (subclavian) arteries down through a subcutaneous tunnel along the side of the torso and anastamose it into both femoral arteries with an upside down “Y” shaped graft arrangement. This procedure, enjoyed so by vascular surgeons, is called an axillo bifemoral bypass, or, an “ax-bi-fem.” In cases of complete aortic obstruction, this is a good surgery to bring blood to the lower extremities to keep them going. The option of bilateral leg amputations empowers one to pursue such creative options.
Western medicine interventions of this sort are often dramatic and very helpful. However, there is much more to consider in terms of the biochemical causes of the underlying pathology.
How does such advanced pathology arise inside of blood vessels and other tissues?
An informative and helpful article on Vitamin K2 recently appeared on Designs for Health’s Research and Education Blog. This writing offers some insight into the biochemistry of calcified tissues, and the importance of vitamin K2 in preventing this common problem.
The Crucial Role of Vitamin K2
“Often, the first thing that come to mind regarding vitamin K is that it comes from leafy greens and has something to do with blood clotting. This fact actually only pertain to vitamin K1, and is a small part of the much larger story of vitamin K.
Vitamin K1 is critical for proper blood clotting. The ‘K’ designation comes from the Danish researcher who first identified its association with ‘koagulation.’ However, while structurally similar to K1, vitamin K2’s physiological function is completely different. K2 serves to direct calcium to the proper organ sites where it needs to be and keeps it out of sites where it causes trouble.
It is telling that there are seemingly paradoxical cases of concurrent osteoporosis and arterial calcification in the same patients. The problem is not too little calcium in the body, but rather, calcium being deposited in the wrong places. There is too little getting into the bones and teeth, and too much being incorrectly shuttled into soft tissue, such as arterial walls, joints, and also precipitating into kidney stones. Vitamin K2 plays a critical role in addressing both of these issues, by activating proteins that direct calcium to the proper destination: Osteocalcin (a.k.a. bone Gla protein) is a marker for osteoblast activity (the building up of new bone tissue), and matrix Gla proteins inhibit the deposition of calcium in the blood vessels. One group of researchers concluded that matrix Gla protein is ‘the strongest inhibitor of tissue calcification presently known.”Both must be carboxylated via vitamin K2 in order to be physiologically active. For this reason, simply supplementing with calcium is not the wisest way to reverse bone loss. Without sufficient K2 to activate these calcium-directing proteins, it would be like throwing fuel on the fire and potentially increasing soft tissue calcification and bone loss.
Just as vitamin D2 is the plant form of vitamin D, while D3 is the form found in animal foods, vitamin K1 comes from the aforementioned leafy greens, but K2 is the form found in animal products. K2 is also produced by bacterial fermentation in some plant foods, such as the traditional Japanese dish of natto—fermented soybeans. Beneficial bacteria in human intestines also produce K2, but the amount may not be sufficient to meet the body’s needs.
The largest source of K2 in the Western diet is fatty cuts (plus dairy fat) of ruminant animals—specifically, ruminant animals that consume their natural diets of grass and hay. Ruminant animals concentrate and bioconvert the K1 in grasses into the K2 that ultimately ends up in cheese, yogurt, butter, fatty meats, and organ meat (liver, in particular). It is also found in egg yolks from hens living in pasture, where they consume grasses as well.
Vitamin K2 is relatively low in the modern American diet. The disappearance of this critical nutrient from our food supply is due to two main factors: the misguided, yet longstanding, emphasis on low-fat and fat-free dairy products; and the factory feedlot system. As the vitamin K2 in animal fats initially comes from the K1 in grass, animals consuming corn, soy, and other feedlot rations do not get the concentrated amount of K1 they would if they were grass-finished, resulting in far less K2 ultimately ending up in their meat and milk.
It’s interesting that more heart attacks seem to occur in winter than summer. We tend to associate this with middle-aged men overexerting themselves while shoveling snow. Granted, shoveling snow is more physically demanding than mowing a lawn, but there is another theory worth considering: vitamin K2 may be more abundant in the food supply during summer, with dairy animals feeding on fresh grass more than in winter. More K2 in the diet could lead to less calcification of coronary arteries, resulting in a lowered risk of coronary events during summer.
When patients present with calcium-related issues—particularly the ‘paradox’ of reduced bone mineral density along with soft tissue calcification—consider vitamin K2 supplementation, as well as encouraging patients to seek out meat and dairy from grass-fed animals.”
Vitamin K2…Additional Information
The linked references in this article should serve to convince you that there has been ample study on the importance of vitamin K2’s role in preventing soft tissue calcification which is a prevalent dynamic in the aging process.
Some additional information on vitamin K2 is presented below.
A common misconception is that vitamins K1 and K2 are simply different forms of the same vitamin with the same physiological functions. However, this is not the case.
All of the K vitamins have similar functions in the clotting cascade. This similarity is related to the part of the vitamin called the naphthoquinone ring structure. This ring structure is identical for both K1 and K2. The two vitamins are only different in their side chains.
The first meaningful study on vitamin K2 was the Rotterdam study, published in 2004. This was the first study of 4800 Dutch people over 7 years demonstrated the beneficial effects of vitamin K2. The Rotterdam Study showed that those who consumed the greatest amounts of K2 had the lowest risk of cardiovascular disease, cardiovascular calcification, and the lowest chance of dying from cardiovascular disease. This study then opened a valuable research window into vitamin K2’s expanding roles. This vitamin is as vital and important for our health as vitamin D.
While K1 is preferentially used by the liver to activate blood clotting proteins, K2 is preferentially used by other tissues to deposit calcium in appropriate locations, such as in the bones and teeth, and prevent it from being pathologically deposited in locations where it does not belong, such as in soft tissue sites.
The concluding remarks in the last article cited above about “paradoxical calcification” is an important concept to note because this particular paradoxical pathology is very common in our western societies…”Vitamin K2 deficiency has recently been recognized as a protagonist in the development of vascular calcification and osteoporosis.” This short abstract is worth reading in its entirety. Furthermore, notation is made of vitamin K2’s influence in regulating cell growth dynamics; an important aspect of cellular differentiation and division which has been noted by other authors.
There are 3 types of vitamin K:
- Vitamin K1, or phylloquinone, is found naturally in plants, especially green vegetables. K1 goes directly to your liver and helps maintain healthy blood clotting. Only about 10% of the vitamin K1 in food is absorbed. Most of our vitamin K1 is synthesized in the intestinal tract by friendly bacteria.
- Vitamin K2, also called menaquinone, is made by the bacteria of the gastrointestinal tract. K2 goes straight to your blood vessel walls, bones, and tissues other than liver.
- Vitamin K3, or menadione, is a synthetic form which is not recommended. Toxicity has occurred in infants injected with this synthetic vitamin K3.
Vitamin K1 does convert into vitamin K2, but this conversion is too inefficient to supply adequate vitamin K2. Furthermore, vitamin K2 is synthesized in the intestines to a small degree, but this intestinal synthesis is only a minor source of this critical nutrient.
Vitamin K1 participates in blood clotting cascades. Vitamin K2 also participates in blood clotting cascades, but to a lesser extent. Its more important role is to help move calcium into bones and teeth by activating the tissue matrix Gla protein and the bone osteoblastic Gla protein (osteocalcin). It may also play a role in removing calcium from areas where it shouldn’t be, such as in arteries and soft tissues. Future research will establish, or discredit, this hypothesis.
Furthermore, vitamin K2 exists in 2 forms:
- MK-4 (menaquinone-4), a short-chain form of vitamin K2 found in animal foods, and is highly bioavailable, but has a short half life in the body.
- MK-7 (menaquinone-7)…a long-chain form found in fermented foods. There is a variety of these long-chain forms but the most common one is MK-7. MK-7 has a longer half life.
The optimal amount of vitamin K2 to ingest on a daily basis is still under investigation. While the ideal dosage has yet to be determined, studies suggest that a dosing of 360-500 micrograms of vitamin K2 per day may be optimal. As evidenced in the Rotterdam Study, 45 mcgs per day will help prevent cardiovascular disease. In this study, people who consumed 45 mcg of K2 daily lived seven years longer than people getting 12 mcg per day.
Because vitamin K2 is not stored in the body like other fat soluble vitamins, it requires daily dosing for optimal function. This is a rather important point. The fat soluble vitamins are A, D, E, and the K family. I recommend that these vitamins be consumed with some sort of fat to enhance their absorption.
It is estimated that up to 80 percent of Americans do not get enough vitamin K2 in their diet to activate their K2 proteins. This is similar to the deficiency rate of vitamin D. However, based on a number of other sources I have read, I believe that the real deficiency incidence may be higher than 95%.
Sources of vitamin K2
While humans have the ability to convert vitamin K1 to vitamin K2, a significant amount of evidence suggests that humans require more preformed K2 in the diet to obtain and maintain optimal health.
As one of the article links above denotes in a tabulated form, some of the foods which are high in vitamin K2 include natto, hard cheese, soft cheese, egg yolks, butter, liver, salami, chicken, ground beef, and other fermented foods such as sauerkraut, kimchi, and kefir.
Vitamin K2 is also available in supplement form. It is appropriately complexed with vitamin D in good vitamin D products. If the vitamin D is not complexed with vitamin K2 then the calcium transport protein will not be properly activated to move the calcium into bones.
Vitamin D and K products which I recommend are offered by Designs for Health and include:
Of special note, Vitamin K2 is also available in another of the DFH products called Tri-K.
The Tri-K formulation contains:
- 2000 mcg Vitamin K1 -the naturally occurring form of vitamin K in vegetables.
- 500 mcg Vitamin K2- in the MK-4 highly bioavailable form. Antibiotics in the food supply reduce the intestinal bacteria that produces vitamin K2. Also, poor conversion of K1 to K2 in some people makes supplementation with K2 (MK-4) important.
- 17.5 mg of trans-geranylgeraniol which supports vitamin K status in the body.
Because vitamin K2 deficiency is so common and is causative to so much important pathology in our culture, I am now recommending Tri-K to almost all clients. Comments about vitamin K2 toxicity follow next.
Because there is no known toxicity of vitamin K1 and K2 and because the diseases associated with vitamin K2 deficiency are so common and so morbid, I recommend to most of my clients to use 1 or 2 capsules/day to enhance strong bones and teeth and help move calcium away from soft tissue deposition in arterial walls and joints and the other sites mentioned.
Measuring vitamin K2 in the serum is influenced by dietary intake and vitamin K2 decay, and may not reveal an accurate assessment of levels. Lab assay by enzyme-linked immunosorbent assays (ELISA) has been developed. These blood tests measure the active and inactive forms of matrix Gla protein. By that, you can more accurately determine whether you’re sufficient in vitamin K or not. These tests should be available in both Europe and the USA in 2015.
Because of the high amounts of vitamin K1 in the Tri-K formula, its use alongside the anticoagulant warfarin (Coumadin), which acts by inhibiting vitamin K1 recycling and thus prolongs clotting times, must be carefully considered. Physicians usually tell their patients who are on Coumadin to avoid consuming the healthy vitamin K1 foods. Patients are told this so that their clotting times can be more easily controlled. However, physicians who want their patients on Coumadin to reduce vitamin K1, but who encourage consumption of green vegetables for their known health benefits, will simply increase the Coumadin dose to acheive therapeutic prolongation of the clotting time.
My medical school pathology teachers taught us back in the 1970’s that early coronary arterial calcification was noted in post mortem examination of 20 year old soldiers killed in the Korean war crisis. This fact is often cited in the halls of medicine, and more recent studies confirm this. In the near future it may also be cited that an important nutritional practice would be to begin vitamin D and vitamin K2 supplementation in early life to help prevent this common problem.
Furthermore, I am discovering from genomics studies that genetic mutations of the Vitamin D Receptor (VDR) of the heterozygous and homozygous forms are rather common. In those who carry these mutations, this means that the vitamin D receptor is not as efficient in its host of critical activities.
The vitamin D receptor (also known as the calcitrol receptor) is a member of the nuclear receptor superfamily and plays a central role in the biological actions of vitamin D. VDR regulates the expression of numerous genes involved in calcium/phosphate homeostasis, cellular proliferation and differentiation, immune response, and other important vitamin D related activities.
The incidence of VDR heterozygous mutation (a mutated gene inherited from one parent) is as high as 43%. The incidence of VDR homozygous mutation (a mutated gene is inherited from both parents) is as high as 10%. Mutated vitamin D receptors mean that the activity at the receptor is not optimal, and more vitamin D will be needed to promote vitamin D’s many health effects.
Matrix Gla protein genetic mutation has been investigated and mutations of this gene are directly associated with coronary arterial calcification.
Furthermore, vitamin K2 is transported in the body via the LDL particles in our cholesterol sub-populations. This may help explain the accumulating observations about those who are on LDL lowering statin drugs and still have progressive coronary atherosclerosis, as well as diminished bone mineralization.
Perhaps what these people really need is vitamin K2, and not so much harmful statin drug usage…such a novel thought.
Statin drugs have harmful side effects and are being over-prescribed by physicians who are not considering negative biochemical side effects such as CoQ10 depletion in the mitochondria, diabetes, and brain decline. It is also known that statin drugs inhibit our body’s endogenous ability to synthesize vitamin K2. See references #4 and 5 below.
Here are several links to associated articles posted in this Journal in the past on the important related subjects of vitamin D and calcium:
Like vitamin D, the importance of vitamin K2 will become more widely recognized and accepted for its important role in health.
Signing off from Crestone and Beyond
Associated Readings:
- Dietary Intake of Menaquinone is Associated with a Reduced Risk of Coronary Heart Disease: The Rotterdam Study…this now famous study was conducted on residents of Rotterdam between 1990 and 1993. Results were reported in 2004, as seen here.
- VitaminK2.org…a website devoted to vitamin K2 research and information
- Vitamin K: an old vitamin in a new perspective…from the Journal of Dermato-Endocrinology, October 30, 2014, is a definitive article which explains a lot of vitamin K biochemistry including the pathology of co-existing arterial calcification and osteoporosis.
- New study recommends statin use for the primary prevention of cardiovascular disease…a new study from 11-14-16, published in JAMA calls for the use of statins in a preventative fashion. The authors advocate the use of low-to-moderate-dose statins in adults ages 40 to 75 years without a history of cardiovascular disease (CVD) who have one or more CVD risk factors (dyslipidemia, diabetes, hypertension, or smoking) and a calculated 10-year CVD event risk of 10% or greater. Read this article to understand the mistaken thinking about what is being promoted here, and the other important concerns, such as vitamin K2, which the medical industry ignores. Regarding the problems that statins cause for vitamin K2 production, see comments in #5 below.
- Statin Drugs: Worse Than We Thought?…an important summary, especially for those who are using statin drugs, posted here on May 12, 2017.
- New study demonstrates importance of vitamin K and cardiovascular function in teens…the importance of vitamin K1 is covered here.
- New review investigates magnesium levels on vitamin D’s effectiveness…the important relationship of magnesium and vitamin D is presented once again in this summary.
- Butter is Beautiful…the value of butter in assisting with your vitamin K2 needs, plus other nice information about butter.
- Introducing the ‘K’ Family…a nice introduction to the vitamin K family and its benefits in our health.
- Osteoporosis is Scurvy of the Bone…Dr. Suzanne Humphries, M.D., registers and explains some biochemistry in this writing which explains the role of vitamin K2, vitamin C, and magnesium in bone health. The deleterious use of excess calcium is also covered.
- New study investigates the role of vitamin K in mobility and disability in older adults…posted here on 6-23-19, this summary is about the role of vitamin K1 and its association with mobility and disability in aging people.
- Multiple Vitamin K Forms Exist in Dairy Foods…researchers from Tufts University herald dairy products as a very good source of vitamin K2. The adequate intake for vitamin K2 is 90 mcg/d for women and 120 mcg/d for men. A one-ounce serving of soft cheese (28 g) provides about 140 mcg of K2—more than the adequate intake for both men and women. It’s important to note that the K2 is mostly present in dairy fat. This explains why the researchers found that low-fat and non-fat dairy products contain only 5 to 22 percent of the K2 that full-fat dairy products contain. In this 2017 study, the authors conclude, “To the best of our knowledge, this is the first report of menaquinone contents of US dairy products. Findings indicate that the amount of vitamin K contents in dairy products is high and proportional to the fat content of the product.”
- Vitamin D for Bones: More is Not Always Better…excellent thinking here about the importance of using vitamin K2, magnesium, and adequate protein intake when supplementing with vitamin D to support bone health. This is an insightful reading. Posted on 1-26-20.
- Vitamin K2: What You May Not Know About This Versatile Molecule…posted here on 3-5-21. A nice summary of vitamin K2. Newly recognized benefits are described.
- Vitamin K2 and GG Mitigate Insulin Resistance by Improving Mitochondrial Function…”Considering dietary vitamin K2 intake is insufficient in the standard American diet or in Western pattern diets, supplementation may not only support mitochondrial and musculoskeletal health, but it may also contribute to healthy blood sugar regulation.” The term GG refers to geranylgeraniol which is a good supplement to use for more graceful aging.