This Journal presents information about butyrate, an essential molecule for a healthy life. Butyrate acts in the intestines to facilitate a variety of important health processes. This Journal extends into general considerations and specifics about gastrointestinal healing. Without a healthy gastrointestinal tract there will not be health in the body, and I daresay there will not be health in the body-mind-emotion-spirit complex that we are.
The Crestone and Beyond collection of writings has been deficient in articles about intestinal health. This consideration has been mentioned sparingly. This Journal entry is an attempt to rectify this lack. Intestinal health is the foundation of overall good health, and so this writing may be overdue.
In his time 2400 years ago Hippocrates said that all diseases begin in the gut. The last several decades of medical research have come around to showing this to be true. Hippocrates also said, “Let your food be your medicine and let your medicine be your food.” This important maxim is also true. The ages old medical system of Ayurveda, which has its origins in India some 500-1000 years before Hippocrates, also expounds the foundational premise of food’s essential role in our health.
I’ll open the website’s coverage of intestinal health by focusing on a single essential gut health molecule known as butyrate. From consideration of this molecule, much can be learned about the basics of intestinal health, and much benefit can be accrued by insuring that one has good butyrate levels in one’s intestinal tract. This writing will also refer to butyrate as butyric acid. The 2 terms are synonymous.
The most important one single molecule for intestinal health that is known is the 4 carbon short-chain fatty acid (SCFA) known as butyrate. It is made from bacterial fermentation and breakdown of the fiber that we eat. It turns out to be the main fuel source for the cells lining the colon wall. If the colonocytes are healthy, then we will be able to enjoy good health in all organ systems.
Being the primary energy source for the colonocytes, butyrate provides up to 70% of their energy needs. And its benefits go far beyond just fueling those cells. Butyrate also reduces inflammation, strengthens the gut barrier, and supports immune system balance. These properties make butyrate a promising molecule for managing a wide variety of conditions and improving overall health.
Disease conditions associated with low butyrate levels include all inflammatory bowel diseases, colon and rectal cancers, metabolic disorders, neurodegenerative conditions, and immune system disorders. Immune system disorders includes all autoimmune disorders of which there are now over 80 different kinds. Autoimmune conditions have their origin in diseased leaky epithelial barriers. I will focus comments on autoimmune disorders in my comments section below.
Our ability to produce butyrate depends on the health of a complex ecosystem of beneficial bacteria in the gut. Both environmental toxins and poor dietary choices can disrupt this microbial balance, reducing the gut’s capacity to ferment fiber and generate butyrate. Such toxins compromise the protective effects that butyrate provides.
In an article which appeared on the March 10, 2025 edition of the Mercola website, Dr. Joseph Mercola, D.O. explores a few features of this virtuoso molecule in an informative and succinct writing. There are a few technical terms which should not deter your reading.
The article is entitled Butyrate–Fueling a Normal Gut Environment and Supporting Energy Production and appears below. The article’s many references are listed below this entry.
Please enjoy and learn from this nice summary about the importance of butyrate. This important information cannot be written more succinctly, clearly, and comprehensively. I’ll add closing considerations. This lengthy Journal is 2 articles in one, with one article supporting the information in the other one.
Here is the Mercola writing.
- Butyrate is an essential short-chain fatty acid (SCFA) that fuels colon cells, supports gut barrier function and promotes a balanced microbiome. Colon cells rely on butyrate for up to 80% of their energy needs, helping maintain normal gut function and a healthy intestinal lining
- Your gut bacteria produce butyrate by fermenting fiber from whole foods such as fruits, vegetables, legumes and whole grains
- Butyrate supports gut barrier integrity by regulating tight-junction proteins and contributing to mucus production, which protects the colon wall
- Diet and lifestyle significantly impact butyrate production — a high-fiber diet, exercise, hydration, sleep and avoiding processed fats all support SCFA production
- Common misconceptions about butyrate include the idea that fiber supplements alone suffice — whole foods provide a wider variety of fiber, nutrients and benefits. If gut health is compromised, gradual fiber introduction is key — eliminating gut-damaging factors first allows for better microbial balance and butyrate production
You might have heard that fiber is good for your gut, and there is a straightforward reason for that advice: certain substances called short-chain fatty acids, or SCFAs. One SCFA in particular, butyrate, often appears in discussions about normal colon function and everyday energy metabolism in the cells that line your colon.
This article provides an overview of butyrate’s role in a balanced gut environment. It also describes how butyrate is made, ways to support its production, and practical points for anyone who wants to improve their digestive function.
What Is Butyrate?
Butyrate, also known as butyric acid, forms in your colon (the lower part of your intestinal tract) when certain bacteria ferment dietary fiber. This process yields several SCFAs, including acetate, propionate and butyrate, which feed your gut microbes and play roles in everyday colon function. Researchers often place special emphasis on butyrate because it serves as a notable energy source for cells in your large intestine.1
•How butyrate is produced in the gut — When you eat fiber-rich foods, say an apple or a serving of legumes, the bulk of the fiber in these foods passes intact through the upper part of your digestive tract. Once it reaches your colon, certain microbes — such as Roseburia or Faecalibacterium — begin to ferment that fiber, thereby generating SCFAs.2
•Butyrate as a vital energy source for colon cells — Colon cells, known as colonocytes, rely on SCFAs for their day-to-day energy needs. Butyrate is a key fuel for these cells. Colonocytes convert the butyrate into an energy carrier called acetyl-CoA, which then enters the Krebs cycle in the mitochondria, resulting in the production of ATP — the energy currency that cells use for just about everything.
•The majority of colonocyte energy comes from butyrate — Research suggests that colonocytes derive anywhere from 70% to 80% of their energy needs from butyrate alone. When colonocytes have a consistent, reliable source of fuel, they’re better able to keep your gut functioning in a normal, efficient manner.
•Butyrate supports vital gut functions — Though there is variation across different populations and dietary patterns, researchers have noted that colonocytes often draw heavily from butyrate to support routine activities, such as fluid exchange with the bloodstream and the upkeep of the gut lining.
To learn more about the broader benefits of butyrate and its impact on overall health, read “Understanding Butyrate — The Key to Optimal Health and Well-Being.”
How Butyrate Supports Your Healthy Gut Barrier
Your intestines, especially the large intestine, have a barrier that helps regulate what passes from the digestive tract into the bloodstream. SCFAs influence molecules known as tight-junction proteins, which act as gatekeepers between cells in your intestinal lining.
•Butyrate strengthens intestinal tight-junction proteins — These proteins include zonula occludens (ZO-1), occludin and claudins, all of which appear in discussions about typical gut barrier function. According to studies, butyrate promotes the normal expression of those proteins, reinforcing intestinal integrity.3
•Butyrate supports mucus production — Scientists have also looked at butyrate’s effect on the mucus layer that coats your colon. Colon cells that function in a normal way contribute to the production of mucus along the interior gut wall. This mucus eases the passage of waste and supports a balanced microbial environment.
•Oxygen reduction and anaerobic bacteria balance — As colonocytes metabolize butyrate, they also consume oxygen in the process, and this is a very good thing.
This process lowers the local oxygen levels in your colon, which in turn allows anaerobic bacteria — beneficial microbes that thrive in low-oxygen environments — to flourish. Some of these bacteria help produce even more SCFAs, creating a beneficial feedback loop that supports and balances your gut microbiome.
Learn more about butyrate’s role in your gut health and metabolism in “Butyrate — The Metabolic Powerhouse Fueling the Gut and Beyond.”
How Do Diet and Lifestyle Influence Butyrate Production?
Dietary fiber stands out as the most obvious step if you want to encourage SCFA production in your gut. By eating foods such as organic whole grains, fruits, vegetables, legumes and other plant-based staples, you provide the fermentable substrates your gut microbes need.4
•Include a wide variety of fiber sources — Ideally, you want to include a wide variety of fiber sources, both soluble and insoluble, as different types of fiber are fermented to varying degrees. Over time, this variety ensures a broader range of benefits for your gut environment.
•Increase fiber intake gradually to prevent bloating — if you’re not used to a high-fiber diet, ramping up too quickly can lead to bloating or gas. A slow increase allows your gut environment to adapt gradually, helping you stay comfortable while you boost butyrate production. Hydration is also important. Without adequate fluids, a high-fiber diet results in constipation.
•Avoid diets high in polyunsaturated fats (PUFAs) — Keep in mind that diets high in polyunsaturated fats (PUFAs), especially those rich in linoleic acid, such as soybean and corn oil, have been shown to shift the microbial balance in ways that undermine SCFA production. So, you’ll want to avoid these fats as much as possible to promote a healthy gut environment.5
•Exercise supports microbial diversity — Aside from diet, physical exercise is also associated with a more diverse microbiome and has a positive impact on gut transit time (how quickly food moves through your digestive system).6
•Sleep and stress impact gut health — Sleep is another lifestyle factor that has an impact on gut health. Sleep deprivation and high stress disrupt your gut microbiome. Prioritizing adequate rest, aiming for seven to eight hours per night, and finding effective stress management techniques (like mindfulness, exercise or hobbies) help maintain a stable internal environment that supports the growth of beneficial SCFA-producing bacteria.7
•Antibiotics affect microbial balance — Antibiotics also deserve attention since they kill off both harmful and beneficial bacteria.8 If you receive an antibiotic prescription, be sure to add some probiotic- or prebiotic-rich foods to help reseed your gut with healthy microbes. Foods such as yogurt, kefir, kimchi or sauerkraut contain microorganisms or compounds that support microbial diversity.
By making these mindful choices in your diet and lifestyle, you create a gut environment that supports butyrate production and enhances overall health.
Common Misconceptions About Butyrate
Butyrate is often misunderstood, with many misconceptions surrounding its role in gut health and how it is produced. Some of the most common myths about it include:
•Fiber supplements are not a substitute for whole foods — One common misconception about butyrate is that fiber supplements alone are sufficient. However, common sense will tell you that a single-type fiber supplement cannot mimic or replace the variety and richness of the fiber found in whole foods. Fruits, vegetables, legumes and whole grains also supply a variety of micronutrients and phytochemicals not found in dedicated fiber supplements.
•Not all fats harm gut health — Another myth claims that high-fat diets always disrupt gut health, but the picture is more nuanced. Not all fats are created equal. While certain processed fats, such as trans fats and large amounts of linoleic acid from vegetable oils, disturb your microbial balance, healthier fat sources — like grass fed butter, ghee, tallow and coconut oil — still belong in a gut-friendly diet. The key is moderation and balance.
•Protein does not automatically harm the gut — Some people claim a high-protein diet will automatically disrupt your gut health. It can, if your diet is extremely high in processed meats and lacking in fiber. But a balanced approach — pairing quality protein sources with plenty of vegetables and whole grains — supports a healthy microbial environment.
•Probiotics do not directly introduce butyrate — Another frequent misconception is that probiotics directly introduce butyrate into your gut. In truth, butyrate production is dependent on specific fiber-fermenting microbes. Some probiotic bacteria do not ferment fiber in a way that yields butyrate. That said, certain probiotic strains help create an environment in which beneficial, fiber-fermenting bacteria flourish.9,10
Clearing up these misconceptions allows you to make informed dietary and lifestyle choices that truly support butyrate production and overall gut health.
Five Practical Strategies for Increasing Butyrate Production
Some people see fiber as a chore, but there are many flavorful and delicious ways to raise your fiber intake.
1.Enjoy naturally fiber-rich foods — Fruits like berries or pears are fiber-rich and naturally sweet, and roasted vegetables with spices bring variety to your plate.
2.Avoid certain fibers if gut health is severely compromised — If your gut health is severely compromised, you might need to avoid certain types of fiber temporarily. Before you load up on fiber, your gut needs to be primed and ready.
3.Eliminate key gut disruptors — The first step is to eliminate key culprits damaging your gut, such as linoleic acid, excess estrogen and EMFs, and to focus on restoration of your cellular energy production.
4.Start with low-fiber carbs to support healing — During the initial healing phase, you’ll need to consume carbs to fuel your cellular energy production, but you’ll want to choose carbs that are very low or even completely lacking in fiber at first so that your gut can heal and your microbial population can come into a better balance.
5.Gradually reintroduce fiber — As your gut begins to heal, you can slowly begin to add more fiber to feed your SCFA-producing bacteria.
For more on how to incorporate fiber into your diet and its role in gut health, as well as your genes and cancer risk, read “Study Links Fiber Consumption to Epigenetic Changes with Anticancer Effects.”
Frequently Asked Questions (FAQs) About Butyrate
Q: Can I just supplement with butyrate directly?
A: While butyrate supplements do exist, most people find it more cost-effective and sustainable to encourage their own gut bacteria to produce it by eating a fiber-rich diet. Always talk with a qualified healthcare professional if you’re considering supplements.
Q: Does cooking affect the fiber that produces butyrate?
A: Cooking can change certain aspects of fiber (such as its structure or solubility), but it typically won’t destroy it entirely. Light cooking can sometimes make vegetables easier to digest, so they might actually ferment more efficiently in some cases.
Q: Are there any signs I might be low in butyrate?
A: There’s no simple way to measure “personal butyrate levels” at home. However, if you frequently experience digestive discomfort or have a diet low in fiber, you’re probably not producing as much butyrate as you could. Focus on gradually increasing your fiber intake and talk to a professional if you have ongoing concerns.
Q: Is all fiber good for producing butyrate?
A: Different fibers can produce different amounts and ratios of SCFAs. However, a varied intake of fiber sources is generally recommended to support overall gut health and a balanced microbiome.
You can download a copy of this Mercola article…Download PDF
References for this article:
- 1 Gut. 1987 Oct;28(10):1221–1227
- 2 Environ Microbiol. 2017;19(1):29-41
- 3 J Clin Gastroenterol. 2006 Mar;40(3):235-43
- 4 Cell Metab. 2014 Aug 21;20(5):779–786
- 5 Nutr J. 2014 Jun 17;13:61
- 6 Oxid Med Cell Longev. 2017 Mar 5;2017:3831972
- 7 Sci Rep. 2016;6:35405
- 8 Trends Mol Med. 2016 May 10;22(6):458–478, Figure 2. Antibiotic-Mediated Microbiota Depletion Causes Disease in Multiple Organs
- 9 Nat Rev Gastroenterol Hepatol. 2017;14(8):491-502
- 10 Environ Microbiol. 2014;16(9):2915-2926
Crestone and Beyond
In my earlier time as a general, vascular, and trauma surgeon there were many patients in my practice with gastrointestinal disorders requiring surgical intervention. The repertoire included conditions of every gastrointestinal organ site, from top to bottom, for conditions of the esophagus, stomach, duodenum, small bowel (jejunum and ileum), colon, and rectum. This also included surgeries on organs attached to the intestinal tract which assisted its functions, such as conditions of the gallbladder, bile ducts, pancreas, and liver.
At this time, from 1977 to 2001, the importance of the health of the intestinal lining was beginning to be more comprehensively understood and appreciated. Known inflammatory bowel diseases, such as Crohn’s disease and ulcerative colitis, and the growing number of defined autoimmune disorders were generating growing scrutiny into the biochemistry of gut physiology. More scrutiny, study, and findings were emerging which revealed the importance of the intestinal mucosal lining and the complexities of its intricate chemistry and biology.
The Pathogenesis of Autoimmune Diseases
The science of the gastrointestinal system was found to be very wide ranging in terms of its impact on the body’s systems…from gut microbe ecology to the biochemistry of the intestinal lining cells, to the immune system, on to the central nervous system, and on as well to every other organ system…gut health was being more and more appreciated.
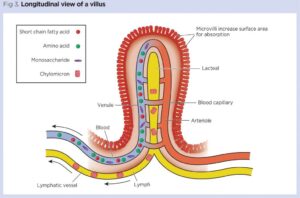
The lining of the intestinal tract is an immense cross sectional area composed of delicate cells known as enterocytes. Fingerlike projections known as villi line the inner bowel wall. The villi are in turn covered by microvilli which is lined by enterocytes. The singular villus and its microvilli serves to increase the cross sectional area for more nutrient absorption.
Enterocytes are susceptible to every type of molecule that comes their way. This vulnerability is the source of toxin absorption into the body, and is also the source of absorption of large food macromolecules which are not supposed to be absorbed. These food macromolecules are the source of autoimmune disorders, of which there are now over 80 different types.
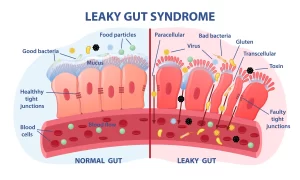
For an autoimmune disease to develop the gut lining integrity is compromised by any of a very wide array of environmental toxins, food borne toxins or opportunistic pathogenic microbial organisms. If these toxins damage the tight junction between enterocytes, then a micro channel between enterocytes opens and unwanted molecules ingress into the circulation of blood. The widened gap space between cells establishes the leaky gut.
Food macromolecules other than normal and healthy carbohydrates, proteins, fats, and elemental vitamins and minerals are recognized by the cells of the immune system. An immune system reaction develops, and is attended by inflammation. The immune system reaction results in the immune cells developing a memory of what this toxin looks like in terms of its 3 dimensional nature and its various chemical signatures.
This immune system reaction to the abnormal molecule establishes a molecular memory of the offending agent. The next step in the autoimmune cascade is the development of molecular mimicry whereby the foreign antigen eliciting the immune system response shares structural similarities with self-antigens; i.e., amino acid sequence similarities between foreign and self-amino acid sequences are enough to result in the cross-activation of autoreactive T or B cells by pathogen-derived peptides.
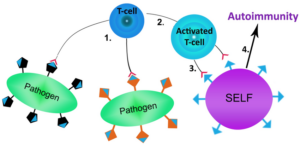
Possessing a new memory feature, the now activated T cells and B cells of the immune system are capable of recognizing amino acid sequences in the protein of our native cell lines. Autoimmunity develops from this activation and attack on native cells lines commences via the process of molecular mimicry.
Autoimmunity Statistics and Types
Susceptible cells lines which are categorized in the generation of the now over 80 different autoimmune diseases include joints, muscles, skin, blood vessels, digestive system, endocrine system, and nervous system.
These diseases affect 1 in 15 people in America. After considering the prevalence of cardiovascular diseases, cancers, type 2 diabetes, and obesity, the rise in autoimmune diseases since WWII is yet another huge concern about the health of Americans. Here is a further look at some statistics of a few of the autoimmune diseases and their prevalence.
- Rheumatoid arthritis affects approximately 1.3 million Americans, making it the third most common type of arthritis after osteoarthritis and gout.
- Psoriasis affects about 3% of the US population which is about 7.5 million people.
- Type 1 diabetes accounts for about 5-10% of all diabetes cases, with an estimated 1.7 million Americans currently diagnosed with this condition.
- Graves’ disease affects about 1 in 100 Americans, making it a leading cause of hyperthyroidism.
- Autoimmune thyroiditis (Hashimoto’s disease), the most common cause of hypothyroidism, affects about five in 100 Americans.
Here is a current listing of the known autoimmune diseases from A to Z.
Some of the more common forms of autoimmunity are seen in this listing from the Cleveland Clinic.
Joints and muscles
Skin and blood vessels
- Sjögren’s syndrome.
- Psoriasis.
- Psoriatic arthritis.
- Dermatomyositis.
- Scleroderma.
- Vasculitis.
- Rheumatoid vasculitis.
- Urticarial vasculitis.
- Vitiligo.
Digestive system
- Crohn’s disease.
- Celiac disease.
- Ulcerative colitis.
- Autoimmune gastritis.
Endocrine system
Nervous system
- Multiple sclerosis (MS).
- Myasthenia gravis (MG).
- Guillain-Barré syndrome.
- Chronic inflammatory demyelinating polyneuropathy (CIPD).
Healing Autoimmunity
The key steps in healing autoimmunity is to remove the offending substances which are being ingested, and to heal the gut lining. The protocol that has been used by most holistically oriented practitioners is called the 4Rs approach:
- Remove Inflammatory Triggers and Pathogens
- Replace Inflammatory Foods with Gut Healing Foods
- Re-inoculate the Gut Microbiota with Beneficial Microbiota
- Repair the Gut Lining

Of course there is a 5th R in a complete gut healing protocol and it is the one that helps tie the 4Rs together. This 5th R is Rebalance. Rebalancing refers to developing balance in sleep health, exercise, and stress reduction techniques. Without helping the nervous system experience of the rest and digest signaling of the parasympathetic nervous system, full attainment of the 4 Rs might be fraught out over a long term with limited success.
Here is a brief and good description of developing the 5 Rs protocol.
Testing for Gut Health
To help guide a more efficient individual gut healing protocol your health practitioner should be using some kind of gut chemistry testing, available from various laboratories, such as:
- GI Effects from Genova Diagnostics
- GI Spotlight from Designs for Health
These kinds of tests reveal a panorama of gut chemistry problems, such as butyrate levels, inflammation chemistry, metabolite imbalance, dysbiosis and microbial ecology balance. Such information will help move gut healing therapy approaches via the 5R protocols forward quickly as the delicate cells of Creation respond to what is right.
In my use of these tests to help evaluate clients’ gut health, I have yet to encounter someone who has healthy butyrate levels! Low butyrate is a very common issue in these times of suboptimal dietary and lifestyle choices and practices.
A Focus on Foods
There are many articles available on the internet which hold forth for a variety of gut healing foods. All of these lists have recommended foods for prebiotic support, probiotic support, and postbiotic support.
Probiotics are foods or supplements that contain live microorganisms intended to maintain or improve the normal good microflora in the body. Probiotics are in foods such as yogurt, kefir, kombucha, sauerkraut, and kimchi.
Prebiotics are typically high-fiber foods that act as food for human microflora. Prebiotics are used with the intention of improving the balance of microorganism ecology. Prebiotics are in foods such as whole grains, bananas, greens, onions, garlic, soybeans, asparagus and artichokes. In addition, probiotics and prebiotics are available as dietary supplements.
Postbiotics refers to the substances left behind after the body digests both prebiotics and probiotics. Healthy postbiotics include nutrients such as butyrate, vitamins B and K, amino acids, and substances called antimicrobial peptides that help to slow down the growth of harmful bacteria.
Here is a short listing of some articles about gut healing foods:
- 12 Foods to Improve Your Gut Health Overnight…fortunately the gut responds to any change rapidly.
- Gut Health Foods: What to Eat and What to Avoid…a listing of 30 foods that help heal as well as foods to avoid in the healing process.
- 20 Foods That Relieve Your Gut Problems, Say Dieticians…a listing of other good foods, most notably bone broths for collagen support.
- Best Foods For Gut Health…a nice little summary of the good foods.
Nutritional Supplement Considerations
The nutritional supplement line I recommend is Designs for Health. This company has the wide array of prebiotics, probiotics, and postbiotics well covered. The entire array of supplements for Gastrointestinal Health is divided into supplements for:
Butyrate and Glutamine
In the Designs for Health (DFH) product line, butyrate is offered as Tri-Butyrin Supreme. This form of butyrate offers 3 types of butyric acid bound to glycerol. Considered to be a postbiotic compound, as mentioned above, butyrate is produced by friendly gut microbes when they break down and ferment dietary fiber. This butyrate supplement may be ideal for those people who cannot tolerate fiber supplements. Here is the Patient Education sheet on Tri-Butyrin Supreme. The starting dose is 1 capsule per day. This delivers 300 mg. of butyrate.
According to this 2020 article, dosage needs for butyrate will vary. “Increased metabolism of the colonocytes in conditions involving intestine damage or inflammation, increased energy expenditure during a disease, stimulation of intestine growth in ‘stress’ conditions with accelerated intestinal passage and increased intestinal excretion, and decreased production of endogenous butyrate due to changes in bacterial flora in different pathological conditions require a significant increase of the supply of this acid.”
A safe dosing schedule is thought to be 300 mg. of butyrate twice daily
The focus of this Journal is on the all important molecule butyrate. However, there are other gut healing molecules. In addition to butyrate, another important gut repair molecule is L-glutamine, an amino acid which serves as a fuel substrate for the cells lining the small bowel where leaky gut and translocation of toxins is also a problem. In serving as a fuel substrate for the enterocytes of the small bowel, this important amino acid helps in enterocyte repair. It is a versatile molecule which also serves the health of the immune system and synthesis of protein for muscle growth and repair.
DFH offers L-glutamine in capsule and powder forms. In addition to the 250 gram powder selection, there is a 500 gram container of identical powder. Here is the Patient Education information on L-glutamine.
Above and beyond these 2 L-glutamine products is the overall gut healing powder formulation offered by DFH…GI Revive powder…a very effective and widely used supplement and recommended to patients by most functional medicine practitioners at some point.
For straight up gut healing, consider GI Revive. For muscle growth and gut healing, consider the L-glutamine products.
Glutamine and butyrate both function as agents to promote health and healing in the small and large bowel lining. Butyrate is very commonly low and so it may be the most important consideration. Glutamine is not commonly low, but boosting its levels in the gut has a nice range of benefits, both in healing the gut lining, and also in supporting other body systems.
Other DFH Supplements for Gut Health and Healing
In addition to butyrate and glutamine, I often recommend a variety of DFH supplements which have proven benefit in gut health, and also in general health.
This list includes prebiotics, probiotics, postbiotics, fiber, vitamins, omega fats, and digestive enzymes.
Examples of some noteworthy DFH prebiotics and probiotics supplements are:
The most important vitamin for gut health is vitamin D. It is a super critical nutrient in all cases of autoimmune disease. It’s levels should be in the high normal range of 60 to 80 ng/ml. Blood levels of vitamin D should be monitored every 6 months; especially in those who are using it therapeutically. A past Journal writing on this vital nutrient is Vitamin D. DFH has this vitamin put up in a nice variety of forms and strengths which you can review on this Vitamin D page.
Omega fatty acids can be reviewed on the Essential Fatty Acid page of the DFH website.
Fiber supplements can be seen on the Fiber page of the DFH website.
Digestive enzyme support is seen on the Digestive Support page of the website.
Conclusion
I often speak with patients about the concept of the “skins” of the body. The body has a collection of organ systems which are lined by skins, or epithelial linings.
Of course, we are all familiar with our outer dermal covering, which we call our skin. But underneath this skin are other skins. In this present Journal writing the focus has been on the skin of the gastrointestinal tract, known as the gastrointestinal epithelium, also known as the mucosal lining of the gut. The other skins to which I am referring here are highly specialized epithelial coverings of the organ structures which they serve. If it is a tube structure in the body, then it is lined by its own specialized inner skin.
You can think of external dermal skin aging as a mirror of internal aging. Skin cells face the same stressors as all other organs. Collagen loss, thinning, and slower healing on our surface skin often reflect deeper cellular strain throughout your body.
Other vital skins whose health is important, and which are susceptible to autoimmune disruption and subsequent disease conditions are:
- blood vessel lining…vascular endothelium
- lymphatic vessel lining
- bronchial and pulmonary lining
- synovial membranes…joint cartilage lining
- urinary tract lining
- hepatobiliary duct lining
- pancreas duct lining
- breast duct lining
- uterus and fallopian tube lining
- brain ventricle lining…ependymal cells
These other skins, as I sometimes call them, abide in their own realms and are sensitive to their own set of toxins and immune system dysfunctions and disease conditions. As such, the human body may be thought of as a system of skins to consider, and to nourish.
An interesting and relevant point is that the central nervous system and our outer skin covering (epidermis) evolve in utero from one of the 3 germ cell layers known as the neuroectoderm. Thus, the brain and the CNS are intimately connected and integrated structures throughout life. Moreover, it is also correct to consider that all of the skins of the body are interconnected and integrated.
I rest this writing by remembering Hippocrates’ 2400 year old admonishment that all diseases start in the intestinal tract. In this writing I have presented some of the basic facts which corroborate Hippocrates’ wisdom that the gastrointestinal tract holds primacy in our health.
“Let your food be your medicine and let your medicine be your food.”
And certain supplements may also be viewed as a very helpful form of food.
Thank you for reading.
Signing off from Crestone and Beyond
Associated Readings
- Is Fiber the New Protein? The Surprising Health Benefits of the Latest Wellness Trend…posted here on 3-4-26. Important points about fiber use are made in this article: “Fiber has replaced protein as the latest wellness obsession, driven by social media trends, food industry marketing and growing concern over gut and metabolic health…Most adults still consume far less fiber than recommended, a gap linked to digestive problems, unstable energy, blood sugar issues and higher chronic disease risk…Fiber improves digestion, heart health, mood and brain function only when the gut environment is healthy, which explains why some people feel better while others feel worse when they increase intake…Adding fiber too quickly or relying on fiber added to ultraprocessed foods often leads to bloating, gas and discomfort, especially in people with existing gut imbalance…The safest way to benefit from fiber is to restore gut stability first, then increase fiber slowly using a wide variety of whole foods while avoiding dietary factors that damage gut and cellular health.”
- A Single Binge-Drinking Episode Can Damage Your Gut…posted here on 2-5-26. There is no amount of alcohol that is safe to consume. Here is another writing that portrays more on this theme. “A single binge-drinking episode triggers rapid immune and barrier damage in your gut, and those changes continue to affect digestion, inflammation, and nutrient absorption for days or weeks afterward…Alcohol causes your immune system to attack your own gut lining, increasing intestinal leakiness and allowing bacterial toxins to enter your bloodstream, which fuels whole-body inflammation…Repeated binge drinking quietly reshapes your gut microbiome, leaving behind a pro-inflammatory bacterial pattern that makes your gut overreact to stress, infection, or irritation long after drinking stops…The gut damage from binge drinking is driven by immune and microbiome disruption, not oxidative stress, which means antioxidants alone do not undo the harm…Even when your gut looks “normal” after drinking, hidden microbial changes remain and raise your risk for inflammation, digestive problems, immune imbalance, and slower recovery when your body is challenged.”
- How Gut Microbiome Imbalances Affect the Health Benefits of Your Diet…posted here on 1-20-26. Main points of this article: “Your gut microbes determine how foods affect your health, meaning identical diets produce very different outcomes on people depending on microbial enzymes, balance, and overall gut condition…Large-scale research shows plant compounds require specific gut microbes for benefits, explaining why plant-heavy diets improve energy for some people yet trigger bloating, fatigue, or food reactions in others…Gut dysbiosis reflects cumulative daily habits, not isolated meals, with ultraprocessed foods, irregular eating, poor sleep, stress, and medications consistently disrupting microbial stability and gut barrier integrity…Sustained lifestyle changes over weeks to months restore healthier microbial activity, improve digestive comfort, reduce inflammation, and support whole-body regulation, especially in people with chronic metabolic or inflammatory issues…Effective gut repair focuses on lowering linoleic acid (LA), gradually restoring carbohydrates, managing stress, improving sleep, and addressing environmental disruptors rather than relying on supplements or one-size-fits-all diet rules.”
- A Deep Dive Into Butyrate–Your Gut’s Powerhouse Molecule…posted here on 1-19-26. The latest Mercola article on butyrate. “Butyrate strengthens your gut barrier, preventing intestinal permeability that allows harmful substances to enter the bloodstream and trigger autoimmune responses…Research shows butyrate improves insulin sensitivity, reduces diabetes risk, lowers bad cholesterol, prevents colorectal cancer, and supports brain health.”
- Your Gut Nervous System Helps Regulate Intestinal Barrier and Allergy Risk…posted here on 12-31-25. The main points covered in this informative article are: “Your gut’s nervous system directly influences whether you tolerate foods or react to them, making it a key factor in food sensitivities and allergy risk…A tiny nerve messenger called the vasoactive intestinal peptide (VIP) tells your gut stem cells how to rebuild the intestinal lining; when VIP drops, your gut produces too many tuft cells that trigger allergy like inflammation…Everyday exposures — like microplastics, seed oils, and emulsifiers found in processed foods — damage tight junction proteins, weaken your gut barrier, and increase the flow of irritants into your bloodstream…Low vitamin D, disrupted sleep, and high stress interfere with your gut’s ability to maintain barrier integrity and calm immune activity, raising your vulnerability to allergic reactions…You can lower your allergy risk by supporting mitochondrial function, removing gut damaging triggers, restoring healthy carbs in the right order, and improving the nerve-gut connection that regulates intestinal healing.”
- Butyrate– The Gut-Brain Axis Connector That Influences Mood and Cognition…posted here on 12-29-25. More on butyrate and its importance in our health. “Butyrate, produced by gut bacteria when they ferment dietary fiber, acts as a signaling molecule in the gut-brain axis, influencing stress, pain tolerance, immunity, and brain health…Through multiple mechanisms, including specific enzyme inhibition and NF-κB pathway regulation, butyrate reduces neuroinflammation and protects against neurodegenerative conditions like Alzheimer’s and Parkinson’s disease…Butyrate influences key neurotransmitters including GABA, serotonin, and dopamine, while also increasing brain-derived neurotrophic factor (BDNF), which supports neuronal growth and cognitive function…The vagus nerve serves as a communication highway between the gut and the brain, transmitting signals about butyrate levels that affect mood regulation, stress response, and immune function…Optimizing gut health through dietary fiber and homemade fermented foods helps promote butyrate production and maintain a healthy gut-brain connection.”
- Butyrate–The Metabolic Powerhouse Fueling the Gut and Beyond…posted here on12-23-25. “Butyrate, a short-chain fatty acid produced by gut bacteria that ferment dietary fiber, helps improve metabolic health by enhancing insulin function, regulating glucose levels, and supporting healthy body composition…Unlike most cells that use glucose, colonocytes (the epithelial cells that line your colon) prefer butyrate for energy, converting 70% to 80% through beta-oxidation to maintain gut barrier health…Promoting butyrate production through fiber intake is beneficial, but only if your gut is healthy. If your gut is compromised, starting with dextrose water before transitioning to whole foods is recommended…Lifestyle factors significantly impact butyrate production, with chronic stress, smoking, excessive drinking and antibiotic overuse reducing beneficial gut bacteria and SCFA production…Excessive linoleic acid consumption, common in processed foods and vegetable oils, reduces beneficial gut bacteria, negatively affecting gut and metabolic health.”
- Butyrate’s Impact on Your Immune System…posted here on 12-15-25. Another good article on butyrate. “Butyrate, a short-chain fatty acid produced when gut bacteria ferment dietary fiber, serves as both an energy source for colon cells and an important signaling molecule for immune regulation…By inhibiting histone deacetylases (HDAC) and suppressing the NF-κB pathway, butyrate acts as a powerful anti-inflammatory agent, helping prevent chronic inflammation that contributes to various diseases…Butyrate promotes regulatory T cell development while modulating other immune cells, helping maintain immune tolerance and preventing autoimmune responses while supporting balanced immune function…Butyrate plays a significant role in managing chronic diseases like IBD, multiple sclerosis and Type 2 diabetes by reducing inflammation and supporting gut barrier function…Emerging research suggests that butyrate influences brain health by modulating the gut-brain axis; it reduces neuroinflammation and supports cognitive function, and plays a supporting role in the prevention of neurological disorders like Alzheimer’s disease and depression.”
- Common Medications Can Disrupt Your Gut Health for Years…posted here on 12-10-25. The main points of this article are: “Researchers from the University of Tartu (in Estonia) found that nearly 90% of 186 common medications affected gut composition, and almost half left long-lasting microbial changes that persisted years after use ended…Antibiotics caused the strongest and most persistent gut disruption, with measurable microbial shifts still evident six months after use and cumulative effects worsening with each additional treatment course…Non-antibiotic drugs like benzodiazepines, beta-blockers, glucocorticoids, and proton pump inhibitors also altered microbial composition…Long-term medication use explained more variation in gut microbiome composition than current prescriptions. This shows that the gut retains a biological “memory” of past pharmaceutical exposures…Restoring gut health starts by reducing unnecessary medications, avoiding vegetable oils, and eating whole foods that help beneficial bacteria recover and rebuild balance over time.”
- Gut Microbes Linked to Stronger Muscles and Healthy Aging…posted here on 11-1-25. This article has some good news. Please read, or at least skim it for its useful and actionable content. Here are the main points: “A new study in Scientific Reports identified specific gut microbes that enhanced grip strength, coordination, and muscle growth in aging mice, increasing muscle weight by over 150% and boosting growth-related markers…Aside from boosting muscle, beneficial microbes improved energy metabolism and reduced inflammation. This helps maintain mitochondrial function and protects against muscle breakdown…Earlier research showed that germ-free mice had smaller, weaker muscles and impaired metabolism, but restoring gut microbes or supplementing short-chain fatty acids (SCFAs) reversed many of these deficits…Nutrition plays a central role in shaping your microbiome. Fiber-rich vegetables, resistant starches, polyphenol-dense fruits, and herbs like red ginseng promote microbial diversity…Beyond diet, other strategies include supplementing with probiotics, prebiotics, synbiotics, and next-generation microbes like Akkermansia, as well as experimental fecal microbiota transplantation (FMT).”
- A Deep Dive Into Butyrate–Your Gut’s Powerhouse Molecule…posted here on 9-30-25. Key points of this article are: “Butyrate is a short-chain fatty acid (SCFA) produced by gut bacteria that ferment dietary fiber. It serves as essential fuel for colon cells and maintaining overall systemic health…Adequate fiber intake — around 30 grams daily — is crucial for butyrate production. Without it, your body burns stored fat and protein, creating disease-causing byproducts…Butyrate strengthens your gut barrier, preventing intestinal permeability that allows harmful substances to enter the bloodstream and trigger autoimmune responses…Research shows butyrate improves insulin sensitivity, reduces diabetes risk, lowers bad cholesterol, prevents colorectal cancer, and supports brain health…Boost butyrate by eating fiber-rich foods, resistant starches, fermented foods and probiotics, while avoiding processed foods, managing stress, and limiting unnecessary antibiotics.”
- How DMSO Heals the Gut and Cures Gastrointestinal Diseases…posted here on 9-11-25. The Midwestern Doctor explains the actions of dimethyl sulfoxide on healthy gastrointestinal disorders. DMSO has a long history as a health agent and over 40,000 studies to back up its efficacy in treating a very wide variety of disorders. Its use was suppressed by the FDA back in the 1970s, but thankfully it is making a comeback.
- What They Don’t Tell You About Autoimmune Disorders…posted here on 8-9-25. The Midwestern Doctor explains on his Substack site. Nicely researched, nicely worded and explained, and comprehensive, as usual.
- LDN Science…a very informative website addressing the use of low dose naltrexone in the treatment of a variety of diseases, including autoimmune diseases. Naltrexone, used for treating opiate dependence, has an off-label repurposed drug role. See this website to learn more about how it has been studied and used to treat autoimmunity.
- Blood Vessel Health, Part I and Part II…a 7-17-23 writing and a 2-14-24 writing on the website about the health of the skin called the vascular endothelium, and how to support it.
- The Central Role of Gut Inflammation in Insulin Resistance…posted here on 7-16-25. “Inflammation in your colon triggers insulin resistance by sending nerve signals from your liver to your pancreas, even before your blood sugar rises…Healing your gut with the right kinds of fiber and eliminating inflammatory foods helps restore beneficial butyrate levels, repair your gut lining and lower your risk for insulin resistance.”
- The Science of Probiotics–How Beneficial Bacteria Support Health…posted here on 6-2-25. Key points made here include: “Gut health is central to overall wellness, with imbalances causing fatigue, weight gain and inflammation across multiple body systems…Combining specific probiotics with plant compounds creates synergistic effects that reduce inflammation and strengthen gut barrier function…Short-chain fatty acids, especially butyrate, strengthen gut lining integrity and regulate immune function, while Akkermansia muciniphila bacteria supports the protective mucus layer where butyrate-producing microbes thrive…Timing matters in gut healing — first remove inflammatory foods like vegetable oils and fix the terrain before gradually introducing fiber and probiotics tailored to your specific condition…Daily habits like avoiding environmental toxins, getting quality sleep and minimizing vegetable oils high in linoleic acid significantly impact microbiome balance and gut health.”
- What They Don’t Tell You About Autoimmune Disorders and Arthritis…posted here on 5-30-25. From A Midwestern Doctor. “This article will review some of the key steps which can be taken to improve autoimmune disorders and reduce one’s reliance upon toxic medications.”
- Unlocking the Secrets of Gut Health…posted here on 4-6-25. “Gut health is key for overall wellness, influencing your immune function, mental health and chronic disease prevention through the complex interactions of your microbiome…Modern lifestyles, characterized by processed foods, antibiotics and environmental toxins, have significantly disrupted gut microbiome diversity, contributing to increased chronic health issues…The delicate balance of gut bacteria depends on maintaining a low-oxygen environment in your colon. Antibiotics and mitochondrial poisons disrupt this balance and promote pathogenic bacterial overgrowth…Restoring gut health requires a holistic approach, including targeted dietary strategies, careful supplementation, stress management and minimizing exposure to environmental toxins like microplastics…Functional medicine emphasizes the interconnectedness of bodily systems, viewing gut health as a fundamental component of overall wellness and a key to preventing chronic diseases.”
- Butyrate–The Gut-Brain Axis Connector That Influences Mood and Cognition…a 3-24-25 Mercola article that explains some of the current research on butyrate’s influence on neurological health. Key points in this article include: “Butyrate, produced by gut bacteria when they ferment dietary fiber, acts as a signaling molecule in the gut-brain axis, influencing stress, pain tolerance, immunity, and brain health…Through multiple mechanisms, including specific enzyme inhibition and NF-κB pathway regulation, butyrate reduces neuroinflammation and protects against neurodegenerative conditions like Alzheimer’s and Parkinson’s disease…Butyrate influences key neurotransmitters including GABA, serotonin, and dopamine, while also increasing brain-derived neurotrophic factor (BDNF), which supports neuronal growth and cognitive function…The vagus nerve serves as a communication highway between the gut and the brain, transmitting signals about butyrate levels that affect mood regulation, stress response, and immune function…Optimizing gut health through dietary fiber and homemade fermented foods helps promote butyrate production and maintain a healthy gut-brain connection.”
- Unlocking Your Gut’s Power to Control Blood Sugar…posted here on 4-3-25 is another informative Mercola article on the importance of gut health. “Short-chain fatty acids (SCFAs) from gut bacteria reduce inflammation and enhance insulin sensitivity, playing a key role in preventing diabetes and metabolic imbalances…Optimizing gut health through mitochondrial support, healthy carbohydrates and targeted supplementation like Akkermansia muciniphila improves glycemic control and overall metabolic function.”
- Gut & Microbiome Health…information and gut healing from the Institute of Functional Medicine.
- Could the probiotic kefir help fight Alzheimer’s disease?…A new study suggests that drinking kefir, a probiotic-rich beverage, may help improve symptoms of Alzheimer’s disease. Researchers believe the beneficial bacteria in kefir could positively influence brain health due to their impact on gut health. While the evidence is still in the early stages, initial results are promising, showing potential improvements in cognitive function and memory for individuals consuming kefir.
- 9 Symptoms of Leaky Gut & What To Do…Amy Myers, MD, weighs in on leaky gut syndrome. This is a nice comprehensive writing on gut health.
- Leaky Gut Syndrome…a nice overview of leaky gut syndrome from the Cleveland Clinic.
- Leaky Gut: What is it, and what does it mean for you?…a Harvard explanation of the problem. This MD writer prefers to end his writing with doubtful words that leaky gut may or may not account for human diseases outside of the intestinal tract. Leaky gut syndrome is still not completely accepted by the status quo medical people, despite the overwhelming evidence and smart thinking by many health care providers.
- Understanding Treatment for Leaky Gut Syndrome…another very good summary of leaky gut syndrome.
- Butyrate’s Impact on Your Immune System…another Mercola article on butyrate from 3-3-25. Some key points include: “By inhibiting histone deacetylases (HDAC) and suppressing the NF-κB pathway, butyrate acts as a powerful anti-inflammatory agent, helping prevent chronic inflammation that contributes to various diseases…Butyrate promotes regulatory T cell development while modulating other immune cells, helping maintain immune tolerance and preventing autoimmune responses while supporting balanced immune function…Butyrate plays a significant role in managing chronic diseases like IBD, multiple sclerosis and Type 2 diabetes by reducing inflammation and supporting gut barrier function…Emerging research suggests that butyrate influences brain health by modulating the gut-brain axis; it reduces neuroinflammation and supports cognitive function, and plays a supporting role in the prevention of neurological disorders like Alzheimer’s disease and depression.”
- Probiotics Offer New Hope for Alzheimer’s and Other Neurodegenerative Diseases…key points of this article include the following: “Probiotics may influence brain function through the gut-brain axis, offering benefits for neurodegenerative diseases like Alzheimer’s and Parkinson’s by improving gut health and reducing inflammation…Studies suggest a link between gut health and cognitive function, indicating that an improved gut microbiome enhances mental health and may reduce inflammation associated with neurodegeneration…Research indicates that probiotics could play a role in managing Alzheimer’s and Parkinson’s, offering a noninvasive treatment option that helps slow or reverse cognitive decline…Biologically, the action of probiotics involves several interconnected pathways. By restoring a healthy balance of gut bacteria, probiotics reduce the production of harmful substances like lipopolysaccharides (LPS) that trigger inflammation in the brain…Further studies are needed to confirm the long-term benefits of probiotics in neurodegenerative disease management, emphasizing the importance of continued research in this area.”
- Leaky Gut Syndrome…a nice overview of leaky gut syndrome from the Cleveland Clinic.
- Leaky Gut: What is it, and what does it mean for you?…a Harvard explanation of the problem. This MD writer prefers to end his writing with doubtful words that leaky gut accounts for human diseases. Leaky gut syndrome is still not completely accepted by the status quo medical people, despite the overwhelming evidence and thinking.
- Integrative Medicine Expert Reveals Links Between Gut Health, Immunity, and Wellness…key points in this Mercola writing include: “Your microbiome plays an important role in training your immune system, with gut dysfunction and increased permeability often leading to autoimmune diseases and inflammation…A healthy colon requires an oxygen-free environment for beneficial bacteria, but environmental toxins and compromised mitochondrial function disrupt this delicate balance…Modern environmental toxins, including microplastics and EMFs, act as mitochondrial poisons, increasing oxygen in the colon and promoting growth of harmful bacteria…Health coaching is a key component of sustainable wellness, providing necessary support and accountability while helping patients implement lasting lifestyle changes…The collaboration between medical professionals, researchers, and health coaches will be key in fostering a health care system that prioritizes holistic, patient-centered care.”
- This molecule links your diet to stroke and Alzheimer’s–here’s how to stop it…an interesting article about the TMAO molecule, where it comes from, and how to mitigate it. “Red meat and eggs feed gut bacteria that make TMAO—a molecule now tied to stroke, Alzheimer’s, and heart failure. This new review reveals how diet, probiotics, and even statins could help stop it in its tracks.” I do not recommend statin use. Instead, use the natural compound that statins are made from, which is Red Yeast Rice.
- How Ginger Helps Alleviate Inflammatory Bowel Disease…posted here on 4-21-25. “Ginger has a long history of soothing digestive issues and modern research confirms its ability to reduce gut inflammation and support intestinal healing…Inflammatory bowel disease (IBD) increases the risk of serious health issues. IBDs like Crohn’s disease and ulcerative colitis cause diarrhea, abdominal pain, and fatigue, increasing the risk of malnutrition, intestinal damage, and colorectal cancer if left untreated.”
- Revolution Health Radio with Chris Kresser on Gut Health…”I unveil the world of Gut Health 3.0, a comprehensive approach that goes far beyond traditional probiotic supplementation. Drawing on the latest scientific research, I explore how polyphenols, bacteriophages, and postbiotics work together to optimize gut health, offering listeners a roadmap to improved digestion, mental clarity, metabolic function, and overall wellness.”
- Gut Microbiome Pattern Helps Predict Heart Attack Risk in Heart Disease Patients…posted here on 5-22-25. “A specific gut microbiome pattern was found to help predict future heart attacks in coronary heart disease patients, offering a new tool beyond cholesterol and blood pressure monitoring…Researchers identified 10 key bacterial strains tied to heart attack risk and created a scoring system that flags high-risk individuals before symptoms appear…Patients with high-risk gut profiles showed more inflammation, insulin resistance, and higher levels of dangerous compounds like trimethylamine N-oxide (TMAO) and endotoxins…Global research confirms gut bacteria influence heart disease through microbial metabolites like short-chain fatty acids, bile acids, and lipopolysaccharide-related immune responses…Natural interventions like berberine, dietary shifts, and fecal transplants show promise in reshaping gut health and reducing cardiovascular risk.”